Responding to Suspected or Confirmed Cases
What do we do when there are confirmed cases?
WHY
To ensure the health of the local community, LEAs may have to take additional measures when a student, teacher, or staff member has symptoms, has been in contact with someone infected, or is diagnosed with COVID-19.
WHAT
Testing for COVID-19
- Recommended: LEAs should recommend testing for students and staff who display symptoms or who have been in close contact with someone who has a confirmed case of COVID-19.
Reporting COVID-19 Cases
- Laboratory Confirmed Cases: Notify the local health department where the workplace is located if there is a laboratory-confirmed case of COVID-19 at the workplace.
- Hospitalization of Staff: Employers should report serious injury, illness, and death, including hospitalization and death from COVID-19, to Cal/OSHA, even if work-relatedness is uncertain.
ISOLATION RECOMMENDATIONS
- Isolation separates those infected with a contagious disease from people who are not infected; and
- Quarantine restricts the movement of persons who were exposed to a contagious disease in case they become infected.
Isolation recommendations
As of December 20, 2021, general CDPH guidance recommends that everyone who has been infected with the virus (regardless of vaccination status or whether they have symptoms) should self-isolate.
Isolation can end after day 5 if:
- Symptoms are not present or are resolving; and
- A diagnostic specimen collected on day 5 or later tests negative.
If unable to test or choosing not to test, and symptoms are not present or are resolving, isolation can end after day 10.
If fever is present, isolation should be continued until fever resolves.
TOOLS
- CDPH’s Decision Tree for managing confirmed or suspected COVID-19 at school
- COVID-19 K-12 Decision Trees from the San Diego COE
RESOURCES
RECOMMENDATIONS FOR STUDENTS EXPOSED TO COVID-19
Schools may consider permitting asymptomatic exposed students, regardless of their COVID-19 vaccination status or location of exposure, to continue to take part in all aspects of K-12 schooling, including sports and extracurricular activities, unless they develop symptoms or test positive for COVID-19.
Recommendations:
- Wear masks for at least 10 days. It is strongly recommended that exposed students wear a well-fitting mask indoors around others for at least 10 days following the date of last exposure, if not already doing so.
- Get tested. Exposed students, regardless of COVID-19 vaccination status, should get tested for COVID-19 with at least one diagnostic test (e.g., an FDA-authorized antigen diagnostic test, PCR diagnostic test, or pooled PCR test) obtained within 3-5 days after last exposure, unless they had COVID-19 within the last 90 days.
- Monitor for symptoms. Exposed students who had COVID-19 within the last 90 days do not need to be tested after exposure but should monitor for symptoms. If symptoms develop, they should isolate and get tested with an antigen test.
- Stay home if tested positive. If the exposed student has symptoms consistent with COVID-19, they should stay home, get tested and follow the Isolation recommendations.
- Follow the Group Tracing Guidance. Schools may follow the recommendations provided in the Group-Tracing Approach to Students Exposed to COVID-19 in a K-12 setting for notification recommendations for exposures that occur in a school setting.
RESOURCES
STAYING HOME AND GETTING TESTED WHEN SICK
Students, teachers, and staff who have symptoms of infectious illness, such as influenza (flu) or COVID-19, should stay home and be referred to their healthcare provider for testing and care. Staying home when sick with COVID-19 is essential to keep COVID-19 infections out of schools and prevent spread to others.
- Follow the strategy for Staying Home when Sick and Getting Tested from the CDC.
- Getting tested for COVID-19 when symptoms are consistent with COVID-19 will help with rapid contact tracing and prevent possible spread at schools.
- Advise staff members and students with symptoms of COVID-19 infection not to return for in-person instruction until they have met CDPH criteria to return to school for those with symptoms:
- At least 24 hours have passed since the resolution of fever without the use of fever-reducing medications; and
- Other symptoms have improved; and
- They have a negative test for SARS-CoV-2, OR a healthcare provider has provided documentation that the symptoms are typical of their underlying chronic condition (e.g., allergies or asthma) OR a healthcare provider has confirmed an alternative named diagnosis (e.g., Streptococcal pharyngitis, Coxsackie virus), OR at least 10 days have passed since symptom onset.
For more information, visit CDPH’s COVID-19 Public Health Guidance for K-12 Schools in California, 2021-22 School Year.
RESOURCES
CONTACT TRACING: INDIVIDUAL AND GROUP-BASED
California’s determination to use every available tool to keep schools safe during this pandemic is allowing us to keep classrooms open and in-school transmission low. Since the start of the pandemic, the state has adapted to new challenges presented and responded with strategies harnessing available tools.
As of January 2022, CDPH has introduced a group-tracing approach as an alternative option for the individual contact tracing requirements in place. Both models are acceptable mitigation strategies to contain transmission of COVID-19 in K-12 schools. However, CDPH strongly recommends that schools utilize (or begin transitioning to) the notification-based model provided in Group-Tracing Approach to Students Exposed to COVID-19 in a K-12 setting.
Other K-12 mitigation strategies remain the same across both frameworks, including recommendations to receive vaccinations and boosters, wear masks indoors, and improve indoor air quality.
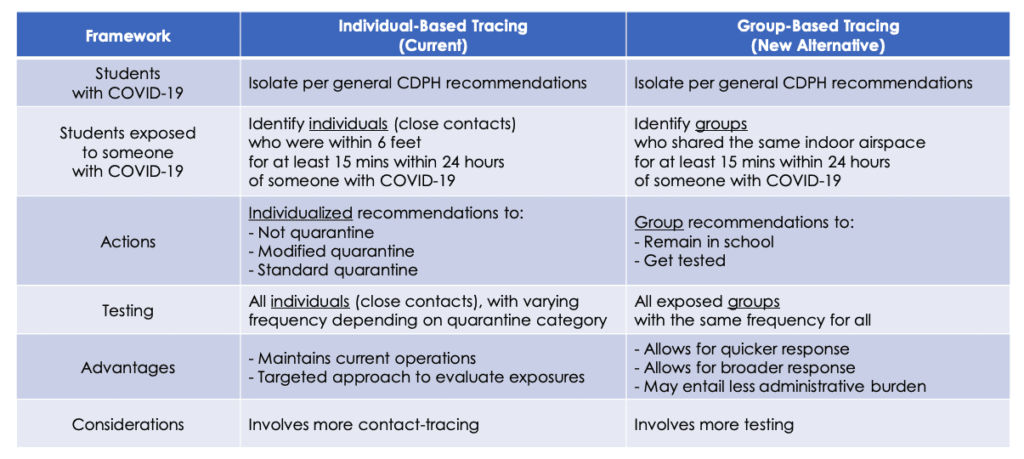
For a high-level comparison between both frameworks, please refer to the Contact Tracing Comparison Summary shown below:
RESOURCES
SCREENING TESTING RECOMMENDATIONS
CDPH has a robust State- and Federally-funded school testing program and subject matter experts available to support school decision-making, including free testing resources to support screening testing programs (software, test kits, shipping, testing, etc.).
Resources for schools interested in testing include:
- California’s Testing Task Force K-12 Schools Testing Program and K-12 school-based COVID-19 testing strategies;
- The Safe Schools for All state technical assistance (TA) portal; and
- the CDC K-12 School Guidance screening testing considerations (in Section 1.4 and Appendix 2) that are specific to the school setting.
REPORTING COVID-19 CASES
The sharing of identified case information data with state and local public health professionals is necessary to ensure that they can respond to confirmed cases of COVID-19 who have been present at a school site, track and understand the extent of disease transmission within the state, and support communities with appropriate prevention strategies and support.
Mandated Reporting
Notify the LHO:
Schools are required to report COVID-19 cases to the local public health department.
Reporting Cases to the Local Health Officer: Schools are required to report COVID-19 cases to the local public health department as per AB 86 (2021) and California Code Title 17, Section 2500.
FERPA Authorization: Schools are authorized under the Family Educational Rights and Privacy Act (FERPA) to disclose personally identifiable information without parental consent to local health departments regarding COVID-19 testing and cases. (20 USC § 1232g(b)(1)(I).)
Notify Cal/OSHA:
LEAs and private schools in California must notify Cal/OSHA of inpatient hospitalizations and deaths among employees, even if work-relatedness is uncertain.
What to Report: For COVID-19, this includes inpatient hospitalizations and deaths among employees, even if work-relatedness is uncertain.
How to Report: Cal/OSHA prefers calls by phone but will also accept email reports that follow the Title 8 section 342 requirements. See the CAL/OSHA guidance for details on reporting and contact information for district offices.
TOOLS
RESOURCES
- COVID-19 Public Health Guidance for K-12 Schools in California, 2021-22 School Year, under Safety Measures for K12 Schools
- Cal/OSHA’s recording and reporting requirements for COVID-19 cases
For more information about how this tool was created and answers to other questions, see the FAQ section.
Last updated on April 6, 2022.




